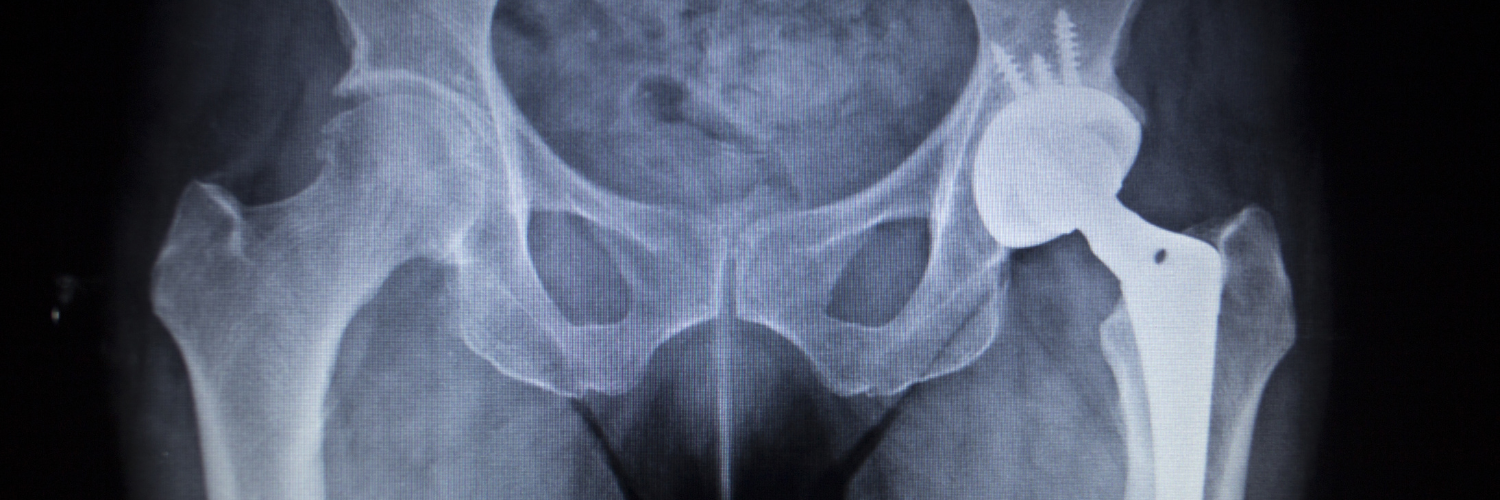
Zero-wait orthopaedics: How Baltic clinics are rescuing UK patients from 18-month NHS agony
For many people living with arthritis, the pain is only part of the struggle. The wait is the real agony. As of early 2026, more than 800,000 people in England are waiting for orthopaedic surgery — hips, knees, and shoulders that no longer move without pain. The NHS’s target of treating 92% of patients within 18 weeks hasn’t been met since 2015. In reality, many wait 18 months or more just to reach an operating table. For some, the delay means living on morphine patches, losing jobs, or giving up independence. For others, it’s simply the fear that their mobility — and dignity — won’t return.
A Baltic alternative
Across the Baltic Sea, the picture looks very different. Clinics in Lithuania, Latvia, Estonia, and Poland are quietly becoming havens for UK patients exhausted by delays. Here, hip and knee replacements can often be arranged in two to six weeks, at half or even a third of the UK’s private prices.
In Kaunas, Lithuania’s medical capital, a network of private orthopaedic centres offers joint replacements for around €5,000–€10,500 (~£4,250–£8,900), including surgery, hospital stay, and rehabilitation. In Riga, Latvia, similar packages include digital pre-assessment and physical therapy follow-up. Rehabilitation is a standard and important part of treatment in the Baltics, with all clinic packages including this aspect to some degree.
Most patients begin with telemedicine consultations, sharing scans and medical histories online. Once approved, they can fly in for surgery within weeks. For recovery, some choose to stay in the region’s rehabilitation clinics or wellness spas — a small silver lining in an otherwise difficult journey.
Stories of relief
The Baltic clinics combine modern facilities, EU medical standards, and streamlined patient pathways. Operations are carried out by internationally trained surgeons, using the same prosthetic components found in British hospitals. Orthopaedic surgeon Sarunas Tarasevicius at Nordclinic in Kaunas told The Sun:
“We have double the patients now from the UK compared to 2019. Most are around 65 and blame waiting lists in the UK. We have people who have been unable to work or walk for two years and have borrowed money for operations here. They have been through so much.”
On patient forums and social media, stories of successful surgeries abroad are multiplying. Many patients share that after being told about several-year long waiting lines with the NHS, they have started looking elsewhere and set their eyes on the Baltic clinics. For example, patient Emma Byrne highly recommends the Polish KCM Clinic after having two surgeries there. In her 5-star review she writes:
“Had such an amazing experience with KCM, this was my second time and yet again the level of care was just amazing. My surgeon went above and beyond with his care I felt in such safe hands. Also can’t thank my patient coordinator Kim enough from the moment I was inquiring about surgery, she was there to talk me through every step.”
Many other reviews praise this clinic – and other Baltic medical centres – for the comfort, extensive pre-operative diagnostic testing, exceptional medical staff and English-speaking support staff.
Intermediaries smooth the path to rapid treatment
When arthritis pain turns every step into an ordeal, waiting another year for treatment feels impossible. Many describe the process as intimidating at first — booking flights, sending scans, navigating foreign paperwork — but ultimately a small price for getting your life back.
Many patients are referred through medical travel brokers, which help coordinate travel, translation, and aftercare. Arturs Lokastovs, a representative from a medical broker agency Treatment in Europe explained the process: “A patient fills out a form on our website, and within 24 hours, we provide offers from several accredited clinics. From there, we guide them through an online consultation and the exchange of medical documents. After a few straightforward steps, most patients are scheduled for surgery within three to six weeks.”
The brokers can also help patients compare the offers and support them with any additional services, if needed – flights, transfers, accommodation, and other needs. It’s worth noting that using a medical travel broker doesn’t necessarily increase the cost for patients. Brokers are typically compensated by the clinics themselves, so the price a patient pays remains the same. If you choose to work with a broker, make sure they operate on this model and don’t add extra fees of their own.
Importantly, patients should take into consideration that the NHS does not reimburse private foreign treatments. Patients choosing not to use a medical travel broker are advised to research thoroughly, check for EU accreditations, and clarify who handles complications or revision surgery back home.
Even so, many who have taken the leap say that when you’re living in constant pain, the reward of walking freely again — within weeks rather than years — makes the journey unquestionably worth it.
Get our free "Ultimate Pre-Treatment Abroad Checklist"
Planning treatment abroad can be overwhelming - but it doesn’t have to be. Our “Ultimate Pre-Treatment Abroad Checklist” guides you step-by-step through everything you need to do before booking your procedure abroad.
A regional boom
Health tourism across Central and Eastern Europe is no longer a niche. Analysts expect the continent’s medical travel market to grow by around 18% a year overall and around 14% in Central and Eastern Europe.
Latvia alone recorded a 16% rise in international medical visitors last year, with patients from the UK leading the charge. Meanwhile, Poland — with its highly accredited private hospitals — now ranks among Europe’s top destinations for elective surgery.
This boom is driven by post-pandemic backlogs, cost-of-living pressures, and a new openness to cross-border care. The EU’s standards for medical devices and hospital accreditation have also strengthened the UK residents’ confidence in the Baltic healthcare systems.
The rise of “zero-wait” orthopaedics in the Baltics is reshaping what access to care looks like.
For some, it’s a lifeline. For others, it’s a worrying sign that the NHS safety net is fraying — and that affordable surgery now depends on a passport and a plane ticket.
Either way, the trend underscores a growing truth: when the system stalls, patients will move — literally — to find relief.
Looking for treatment options? We can help you find the best care abroad in 24-48h!

Get the medical Care You Need at 50–70% Less

EU-Certified Clinics
.svg)
Short waiting time
Get clinic quotes in 24-48h — free & no commitment
What's next?
- Get a quote for procedure
- Consultation with our coordinator
- Confirm the quote
- Arrange your travel


